Why has it proven difficult to stem the obesity epidemic?
Why has it proven difficult to stem the obesity epidemic?
Author: Joseph Proietto
Victoria, Australia
Weight Control Clinic Austin Health Heidelberg
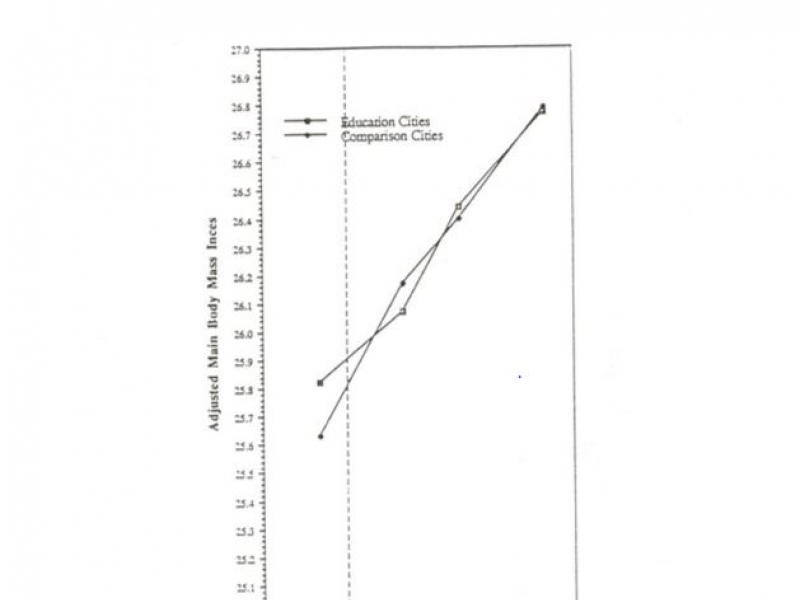
Why has it proven so difficult to stem the obesity epidemic? The most common view is that the cause of obesity is an overabundance of easily available high-energy food and the absence of any obligatory need to be active. What is most surprising however is that educating the population about the causes and significant consequences of obesity, has not resulted in any decrease in the prevalence of obesity. This was clearly demonstrated by the Minnesota heart study (1). This was a long (13 year) study whose aim was to reduce cardiovascular risk. Three intervention cities were compared to three control cities. The interventions were quite comprehensive, including 7 years of community intervention activities that included risk factor screening, mass media education, adult education classes, worksite interventions, home correspondence programs, school-based programs, restaurant programs, and point-of-purchase education in supermarkets. The messages spoke about the benefits of weight loss and the services available to assist people to lose weight. The cohort study showed that this extensive intervention had absolutely no effect on the increase in the prevalence of obesity (Fig 1). The authors concluded that the failure to make any impact on the prevalence of obesity was that for every positive message there were multiple negative ones. Considering the fact that no one wants to be obese, this seems an unsatisfactory explanation. Is there a deeper reason why education alone fails?
A large body of research has found that the brain regulates weight. The mechanism is still being unravelled and the details will not be discussed here. All that we need to know is that in the Arcuate Nucleus of the hypothalamus there are two types of nerves. One type (the NPY nerves) make us hungry and the other (the POMC nerves) take our hunger away. Whether we want to eat or not at any particular time, depends on which of these nerves is firing most. If these are the nerves that determine when we eat, what controls them? There are multiple circulating hormones and nutrients that can influence the drive to eat. Interestingly, the majority inhibit hunger. So far only two hormones, one made in the stomach (Ghrelin) and the other in the colon (ILP5), stimulate hunger. It has been shown that following weight loss, the hunger suppressing hormone leptin decreases (2) and the hunger-inducing hormone ghrelin increases (3) making the individual more hungry following weight loss.
In 2011 it was shown that the levels of multiple hormones and nutrients (e.g ghrelin, leptin, PYY, CCK, Amylin, Insulin, GIP, glucose, FFA) change in a direction to encourage weight regain and that these changes are long lasting (4). In addition after weight loss there is also a drop in energy expenditure (5) that is also long lasting (6).
The fact that weight is defended by the body so vigorously explains why most people have to struggle to maintain weight loss and it also explains why public health measures based on education alone ultimately fail. Even if someone takes note of the information about a healthy lifestyle and they initially succeed in losing some weight, the triggering of the defence mechanism increases hunger and reduces energy expenditure. Before long, food intake increases and weight is regained.
For public health programs to work, it would be necessary to re-engineer society to restrict high-energy food by placing a ban on, or severely taxing, all fatty or high sugar foods and placing the population on energy rationing. Rationing would be essential because it is possible to remain obese by overeating healthy food. In addition, it would be necessary to make physical activity obligatory. This would involve banning the use of cars, restricting use to elevators and escalators and slowing the rapid pace of modern life to allow people to walk to their various meetings. The severe infringement of personal freedom that this would require makes such changes impossible in free democracies. There must be a better way.
How are we to stem the obesity epidemic? There is clear evidence that obesity is either genetic (7-9) or epigenetic (10) as evidence by the studies below. While at present we cannot influence genetic obesity, there is the theoretical possibility that we can prevent epigenetic obesity. To achieve this however requires much research on all of the environmental triggers to obesity including preconception, intrauterine and post-natal causes.
References
- Jeffery RW et al. Evaluation of weight reduction in a community intervention for cardiovascular disease risk: changes in body mass index in the Minnesota heart Health program. Int J Obes Relat Metab Disord 19:30-39 1995
- Geldszus R et al. Serum leptin and weight reduction in female obesity. E J Endocrinol 135:659 1996
- Cummings DE et al Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med 2002 May 23;346(21):1623-30.
- Sumithran P et al. Long term persistence of hormonal adaptations to weight loss. N Engl J Med 365;1597 201
- Leibel RL et al. Changes in energy expenditure resulting from altered body weight. New Engl J Med 332:621 1995
- Rosenbaum M et al. Long term persistence of adaptive thermogenesis in subjects who have maintained a reduced body weight. Am J Clin Nutr 88:906 2008
- Stunkard AJ. et al. The body mass of twins who have been reared apart. N Engl J Med 322:1483 1990
- Bouchard C. The response to long-term overfeeding in identical twins. N Engl J Med 322:1477 1990
- Stunkard AJ. et al An adoption study of human obesity. N Engl J Med 314: 193 1986
- Ravelli GP Obesity in young men after famine exposure in utero and early infancy. N Engl J Med 295:349 1976